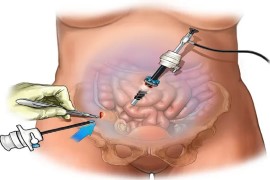
Laparoscopic Colorectal Cancer Surgery
Laparoscopic colorectal cancer surgery, also known as minimally invasive or keyhole surgery, is a surgical technique used to treat colorectal cancer. It involves accessing the abdominal cavity through several small incisions, typically ranging from 0.5 to 1.5 centimeters in size, and using specialized instruments and a laparoscope (a thin, flexible tube with a camera) to perform the surgery. This approach offers several advantages over traditional open surgery, including reduced post-operative pain, smaller incisions, faster recovery times, and shorter hospital stays.
What are the common symptoms of Laparoscopic Colorectal Cancer Surgery?
Laparoscopic colorectal cancer surgery is a minimally invasive surgical technique used to treat colorectal cancer. The common symptoms experienced after laparoscopic colorectal cancer surgery can vary from person to person, but here are some typical symptoms:
- Pain and discomfort
- Incision-related symptoms
- Fatigue
- Changes in bowel movements
- Limited mobility
- Swelling or bloating
- Changes in diet
Types of Laparoscopic Colorectal Cancer Surgery?
Here are some key aspects of laparoscopic colorectal cancer surgery:
- Colectomy: Laparoscopic colectomy is the removal of a portion of the colon affected by colorectal cancer. The extent of the colectomy depends on the location and stage of the cancer. It can range from a segmental colectomy, where only the cancerous portion of the colon is removed, to a total colectomy, where the entire colon is removed. The remaining healthy ends of the colon are then joined together (anastomosis).
- Lymph Node Dissection: During laparoscopic colorectal cancer surgery, nearby lymph nodes are also removed and examined to determine if the cancer has spread. This information helps in staging the cancer and planning further treatment.
- Rectal Cancer Surgery: In cases of rectal cancer, laparoscopic techniques can be used for low anterior resection or total mesorectal excision (TME). These procedures involve the removal of the tumor and a portion of the rectum, along with the surrounding lymph nodes. In some cases, a temporary or permanent colostomy (diverting the bowel through an opening in the abdominal wall) may be necessary.
- Sphincter-Preserving Surgery: When possible, laparoscopic surgery aims to preserve the anal sphincter function by removing the tumor while maintaining bowel continuity and avoiding the need for a permanent colostomy. This is particularly important for rectal cancer surgery.
- Transanal Minimally Invasive Surgery (TAMIS): In certain cases of rectal cancer, TAMIS may be used in conjunction with laparoscopic surgery. TAMIS allows for local excision of small rectal tumors through the anus, complementing the laparoscopic approach.
- Robotic-Assisted Surgery: In some centers, robotic-assisted laparoscopic colorectal cancer surgery may be available. Robotic systems provide enhanced dexterity and precision, allowing surgeons to perform complex maneuvers with more ease. Robotic surgery can be particularly useful for deep pelvic dissections or challenging anatomical situations.
How to prepare for Laparoscopic Colorectal Cancer Surgery?
- Preoperative evaluation: Your healthcare team will conduct a thorough preoperative evaluation, which may include blood tests, imaging scans, colonoscopy, and other tests to assess your overall health and determine the extent of the cancer. This evaluation will help your healthcare team plan the surgery and determine the most appropriate approach.
- Medical history and medications: Provide your healthcare team with a complete and accurate medical history, including any previous surgeries, chronic conditions, and allergies. Inform them about all medications you are currently taking, including prescription medications, over-the-counter drugs, and supplements. They will advise you on which medications to continue or stop before surgery.
- Smoking cessation: If you smoke, it is highly recommended to quit smoking before surgery. Smoking can increase the risk of complications during and after surgery. Talk to your healthcare team about smoking cessation programs or resources to help you quit.
- Medication adjustments: Certain medications, such as blood thinners or antiplatelet drugs, may need to be adjusted or temporarily stopped before surgery to minimize bleeding risks. Follow your healthcare team's instructions regarding medication management leading up to the surgery.
- Bowel preparation: Your healthcare team may provide instructions for bowel preparation before the surgery. This typically involves consuming a clear liquid diet and taking laxatives or bowel-cleansing medications to empty the bowel and reduce the risk of contamination during surgery. Follow the bowel preparation instructions carefully to ensure optimal conditions for the surgery.
- Nutritional evaluation: Adequate nutrition plays a crucial role in the healing process. Your healthcare team may recommend a nutritional evaluation and provide dietary recommendations to optimize your nutritional status before surgery. Follow their guidance regarding diet and nutritional requirements leading up to the surgery.
- Informed consent: You will be asked to provide informed consent for the surgery, indicating that you understand the nature of the procedure, its potential risks and benefits, and the alternatives available. Take the time to discuss any concerns or questions with your healthcare team before signing the consent form.
- Preoperative instructions: Follow any preoperative instructions provided by your healthcare team. This may include fasting guidelines (typically no food or drink after midnight the night before surgery), showering protocols, and specific instructions about medications or supplements to take or avoid.
- Arrange support: Arrange for a support system to assist you before and after surgery. This can involve having a family member or friend accompany you to the hospital, helping with daily activities, and providing emotional support.
Best Doctor For Laparoscopic Colorectal Cancer Surgery In Ahmedabad
Dr. Manthan Merja (Patel)
MBBS, MS (Gen. Surgery) - B. J. Medical College.
MCh-Surgical Oncologist - GCRI, BJMC.
- FIOP (ESSO Europe)
- FARIS (Robotic Surgery)
- FALS (Robotic Surgery)
Dr. Manthan Merja is a consultant surgical oncologist in Ahmedabad. He is a qualified
oncologist with over 10 years of experience in the field. He is an expert in the
treatment of all types of cancer, including breast cancer, lung cancer, colorectal
cancer, and gastric cancer.
Dr. Merja completed his MBBS from BJ Medical College, Ahmedabad in 2012. He then went on
to complete his MS in General Surgery from the same college in 2015. In 2019, he
completed his MCh in Surgical Oncology from Gujarat Cancer & Research Institute.
FAQ About Laparoscopic Colorectal Cancer Surgery
-
What is laparoscopic colorectal cancer surgery?Laparoscopic colorectal cancer surgery is a minimally invasive surgical technique used to treat colorectal cancer. It involves making several small incisions in the abdomen through which a laparoscope (a thin, flexible tube with a camera) and surgical instruments are inserted. This approach allows the surgeon to visualize and access the affected area, remove the cancerous tissue, and potentially perform other necessary procedures.
-
How long does laparoscopic colorectal cancer surgery take?The duration of laparoscopic colorectal cancer surgery can vary depending on factors such as the complexity of the case, the extent of the cancer, and the surgeon's experience. Generally, the surgery can take several hours. However, it is best to consult with your surgeon for a more accurate estimate based on your specific case.
-
Will I be awake during laparoscopic colorectal cancer surgery?No, laparoscopic colorectal cancer surgery is performed under general anesthesia. You will be asleep and will not feel any pain or discomfort during the procedure.